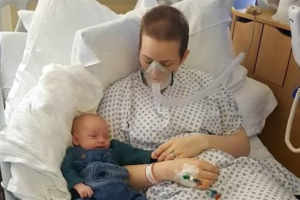
 DES MOINES, Iowa, June 21, 2016 (LifeSiteNews) — Katie Buck felt that any moment she was about to completely lose it as she sat in the hospital room listening to the devastating words of the doctor. The 29-year-old mother suddenly felt as if she was living somebody else’s life, or like she was having a bad dream from which she could not wake up. Her precious newborn baby was going to die. The baby she had carried within her womb for 37 weeks and who she had born into the world just days ago would no longer be there for her to hold, to love, to kiss. She felt her world come crashing down around her.
DES MOINES, Iowa, June 21, 2016 (LifeSiteNews) — Katie Buck felt that any moment she was about to completely lose it as she sat in the hospital room listening to the devastating words of the doctor. The 29-year-old mother suddenly felt as if she was living somebody else’s life, or like she was having a bad dream from which she could not wake up. Her precious newborn baby was going to die. The baby she had carried within her womb for 37 weeks and who she had born into the world just days ago would no longer be there for her to hold, to love, to kiss. She felt her world come crashing down around her.
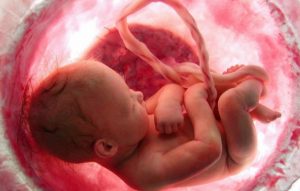
It was just three days prior to this that doctors had decided to induce Katie, even though it was three weeks before her due date. Scans had revealed that her little baby was not developing properly. He was too small. And to make matters worse, the flow of blood through his umbilical cord that delivered life-giving nourishment and oxygen was somehow restricted.

While the birth went well, Katie and her husband Ryan could immediately tell that not all was right with their little boy, whom they had named Alexander before he was born.
“He had some low-set ears. He had an extra thumb. The shape of his head was a little off,” Katie told LifeSiteNews. “You could just tell that something was going on.”
The parents had refused genetic testing earlier in the pregnancy on principle, believing it to be discriminatory against disabled people. They had decided to love and respect any baby that came to them, whether the baby had problems or not.
Blood tests were carried out on the tiny four-and-a-half pound Alexander, but the results were not fast coming. And then, three days after his December 8 birth, the doctor walked into Katie’s room to tell her what the tests had found.
‘Not in his best interest’
Alexander had Trisomy 18, a condition where there are three copies of chromosome 18 instead of the normal two. The condition often disrupts the baby’s normal pattern of development, often causing life-threatening problems including defects in the heart, lungs, kidneys as well as other developmental problems. A large majority of babies with this condition die within the first year.
As she sat now in the Des Moines hospital room listening to the doctor, Katie was having trouble taking it all in. Words became jumbled. It was all too surreal. She asked the doctor to wait until her husband arrived to finish what he had to say.
When Ryan arrived, he found his wife totally distraught. Katie pleaded with him to go with the doctor into another room to discuss Alexander’s condition. When Ryan asked the doctor if he could record what he was about to hear so that his wife could listen to it once she had calmed down, the doctor consented.
What Ryan caught the doctor saying on film six months ago when Alexander was born continues to anger him and his wife to this very day.
“He’s got increased risk of having significant heart defects…rib, kidney abnormalities, inter-abdominal tumors. All of those are not super important because some ninety percent of those kids don’t make it past the first month of age,” the doctor said.
Offering no help and giving no hope, but suggesting death as the only possible outcome for the baby, the doctor continued:
“We can look at his heart and run all kinds of tests, but no matter what his heart shows, heart surgery is not in his best interest, okay? Why put him through a big surgery, cause pain, discomfort, extend his stay if we can get him home? And, his life expectancy isn’t going to be lengthened by a heart surgery.”
Ryan, like his wife, was deeply shaken by the doctor’s words.
“Is there, like, a chance? Is it really that bleak?” he asked.
“It really is,” the doctor replied. “Ninety percent don’t make it through the first year. Most will die in the first month.”
The doctor then went on to tell the shaken father that it didn’t matter if Alexander ate or not, suggesting that if he didn’t eat, “that’s ok too.”
“There is, how do I say it, very little limiting you from going home tomorrow,” he said. “Bottle feed him, breast feed him. Whatever he takes, great. Whatever he doesn’t take, that’s ok too,” the doctor said.
When the dad asked about the possibility of a feeding tube, the doctor immediately questioned the move.
Not giving up
Despite the doctor’s bleak prognosis, the parents did not intend to give up on their baby so easily. They stayed in the hospital another two weeks so that Alexander could receive a feeding tube and so that other tests could be continued.
“He was going to have a full tummy, no matter what happened to him,” Katie said.
But at each new twist or turn, the couple found roadblocks to Alexander’s care. For instance, despite the baby having a heart murmur that was easily picked up during his constant monitoring, no one suggested that he undergo a heart scan to determine the extent of the problem. When Alexander was having trouble breathing, no one suggested that he be hooked up to the oxygen machine.
“Alex actually needed oxygen and they didn’t give him any. We didn’t realize he needed it. We assumed he was ok, that it was perhaps a normal variant for him being born so small. But later we learned that he actually suffered from not having enough oxygen in his blood,” Katie said.
Doctors even suggested that it would be pointless to treat the baby’s case of jaundice. The parents had to constantly argue for tests or treatment that would have been offered to babies with normal chromosomes. When the parents suggested certain tests that might be done on Alexander to determined the extent of his problems, the doctor would say to them, “I just wouldn’t.”
Despite many odds, Alexander was eventually stable enough to go home. But the doctor’s dire words about the boy’s inevitable death kept ringing in the parents’ ears. At every moment, they expected their son to leave them.
“The doctor was the expert,” Katie said. “I really believed him. I wasn’t in a state of denial. I really believed Alex was going to die.”
But Alexander didn’t die.
Days turned into weeks. Weeks turned into months. Time went by and Alexander kept on not only living and growing, but thriving beyond everyone’s expectations.

“It was scary at first because you live as if death is on your doorstep. We were very apprehensive. It was very hard to enjoy a lot of our time with him. We would often think whether or not this was the last time we were going to give him a bath, or was this the last time I was going to breast-feed him, or was this the last time he was going to play with his brother,” Katie said.
When Katie and Ryan saw that Alexander was staying put for the time being, they realized that they needed to stop living in the future of the “what if” and live in the present of the “here and now.”
“Alex has taught me so much about not worrying about tomorrow. All the Scriptures about not worrying about tomorrow, they are true,” said Katie.
It has now been over six months since Alexander returned home from the hospital. The parents have learned how to change his feeding tube, how to administer oxygen, and how to tend for their baby who needs a little more care than other babies.
But most of all, they have learn an important lesson from their son about the beauty of life itself, no matter what kind of package it comes in.
“He rolls, he coos, he smiles. He is very social. He makes a lot of eye contact,” Katie said.
One day the parents were bolstered by a surprise visit in their home from Sen. Rick Santorum, whose eight-year-old daughter Bella also has Trisomy 18. Santorum talked about what a joy Bella is to their family and encouraged Ryan and Katie by telling them that they were doing the right thing.

Santorum gave the family a copy of Bella’s Gift, a book published in 2014 that tells the story of life with their special-needs youngest child. In the book, he inscribed this message:
“To Alex – You are blessed to be born to a family that loves you unconditionally. May God continue to bless you as you bless others who cross your path. Your friend, Rick Santorum.”
Katie remembers being encouraged by Santorum’s visit and his words.

“Alex will continue to surprise you. No matter what happens, everything will be ok,” she remembers him saying.
Full of surprises
And Alexander continues to be full of surprises.
“To be honest, his future is still uncertain, but that is frankly true for any of us. But, there is nothing in his immediate future that is life-threatening,” Katie said.
Katie said that the experience has taught her to be more cautious about what the doctor says, especially when it involves the life of a baby with chromosomal abnormalities.
“There is a pattern of tactics that these doctors use to steer these babies towards death,” she said, adding, “But, they can’t predict the future. They don’t have crystal balls. They can’t say for sure whether your child will live or die.”
Katie was able to tell the doctor to his face what she thought about his attitude toward her son.
“I told him that he made me very uncomfortable when he recommended that we not feed Alex. And I told him that he should strongly consider giving parents all of the options and information, rather than his own opinion, because we are the ones who need to live with these decisions at the end of the day,” she recalled.

Katie and Alex believe that the medical community needs to change its perceptive on babies who have extra chromosomes.
“The belief has been perpetuated that Trisomy 18 means that affected babies are ‘incompatible with life.’ And that is just not true,” said Katie.
“Even if they don’t survive for very long, that is the only life that they have, and it should be respected, treated with dignity, most of all loved, and given just as much care as any other baby would receive. Our children deserve no less,” she said.
Editor’s note: The Buck family has created a gofundme page here to help cover the cost of Alexander’s care. They have also created a facebook page.

 Fr. Shenan Boquet
Fr. Shenan Boquet CAMBRIDGE, Massachusetts, June 19, 2017 (
CAMBRIDGE, Massachusetts, June 19, 2017 (
 (
( by
by 
 Cardinal Carlo Caffarra, archbishop emeritus of Bologna, Italy, has a key message to deliver: Great efforts must be made in Catholic education and catechesis if the Church is to combat today’s attacks on marriage, life and the family.
Cardinal Carlo Caffarra, archbishop emeritus of Bologna, Italy, has a key message to deliver: Great efforts must be made in Catholic education and catechesis if the Church is to combat today’s attacks on marriage, life and the family. June 12, 2017
June 12, 2017  BISHKEK, Kyrgyzstan, May 31, 2017 (
BISHKEK, Kyrgyzstan, May 31, 2017 ( Robert Cardinal Sarah’s recent book
Robert Cardinal Sarah’s recent book 
 The dedication and legacy of a prodigious pro-life hero
The dedication and legacy of a prodigious pro-life hero June 7, 2017 (
June 7, 2017 (
 The Brazilian priest Alexandre Awi Mello, the National Director of Brazil’s Schönstatt Movement, will serve as the new secretary for the the Dicastery for Laity, Family and Life. He was born Rio de Janeiro in 1971, and was ordained a priest in 2001.
The Brazilian priest Alexandre Awi Mello, the National Director of Brazil’s Schönstatt Movement, will serve as the new secretary for the the Dicastery for Laity, Family and Life. He was born Rio de Janeiro in 1971, and was ordained a priest in 2001. Let’s say he lived in Philadelphia in the 1950s. He came from an Italian American family. He sees his Dad, his uncles, his grandfather. They are working class. They sweat in dangerous jobs to support their large families. They come home to a little house full of kids. Its a good life, but its a hard life.
Let’s say he lived in Philadelphia in the 1950s. He came from an Italian American family. He sees his Dad, his uncles, his grandfather. They are working class. They sweat in dangerous jobs to support their large families. They come home to a little house full of kids. Its a good life, but its a hard life.






Hormonal Contraceptives: Do We Really Know What We Think We Know?
Author: Chandler Marrs, PhD
Over the last few years, we have been commission for a two studies on the safety of hormonal contraceptives. One study, the Real Risk project, ended early due to a loss of funding. As a result, Phase 2 data were never analyzed. (We decided to continue collecting data in the hopes of finding funding to complete the study at some point. We haven’t found the funding yet.) Nevertheless, we learned a lot and what we learned should be public. Slowly, some of that information is making its way into blog posts.
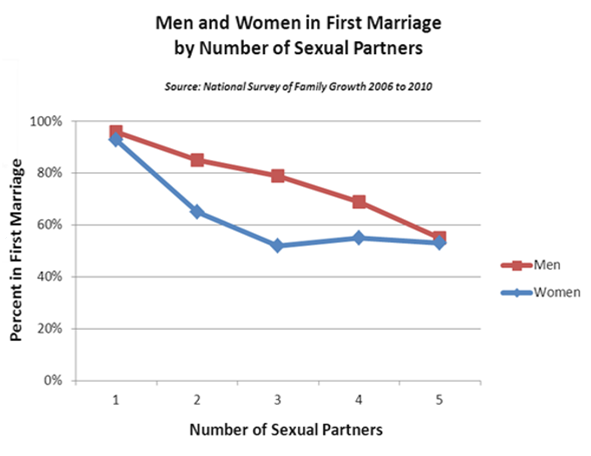
Below is a portion of the final report, covering the history of the pill, a sort of ‘what they knew when’ of side effects. Looking back at the history of the development of the pill and other forms of hormonal contraception, it becomes clear that the health and safety of the female population was not a primary objective. Indeed, more often than not, the serious side effects were ignored, particularly in the US, setting the precedent for the almost total acceptance of the drug’s safety that we see today. As a woman who used hormonal birth control and developed many of the side effects noted by early researchers, side effects that were ignored by my physicians, reading this is eye-opening. If I had known then what I know now, I would have never used this drug.
The History of Birth Control Induced Side Effects
The first case of birth control induced thrombosis, a pulmonary embolism, was reported in 1961, only one year after the drug’s release. This was soon followed by the first contraceptive induced myocardial infarction in 1963. In the years that followed, research groups, primarily in Great Britain, began delineating the risks and mechanisms by which hormonal contraceptives induced the state of hypercoagulability that led to thrombotic events. Much of this research, along with the publication of Barbara Seaman’s book, The Doctor’s Case Against the Pill, formed the impetus for the Nelson Pill Hearings (NPH) in 1970.
Early on, British researchers noted significant changes in blood clotting mechanisms in the women using oral contraceptives compared to those who did not, but also compared to pregnant women. Hormonal birth control, it appeared, increased several pro-clotting factors while simultaneously decreasing anti-clotting factors; changes in hemodynamics that were in many ways, though not entirely, akin to late pregnancy and early postpartum where blood clots are known risks. This was in addition to systemic vessel wall damage that simultaneously set the stage for both clotting and hemorrhage. They also found that clot risk increased over time and was compounded by other variables such as exercise and smoking. In 1967, based upon the results of three studies, the British Medical Research Council issued a preliminary communication that stated:
Politics and Money Rewrite History
These findings, though clearly implicating hormonal contraceptives in thrombosis, became immediately controversial and were all-but-entirely dismissed by American medical societies who argued an inherent difference between British and American women (NPH pages 6222-6259); one that supposedly predisposed British women more strongly towards blood clots than their American counterparts.
Additionally, according to testimony made in the Nelson Pill Hearings, the American Medical Association allowed industry experts to write and publish the early safety statements while simultaneously refusing to publish research and case reports indicative of risk (NPH page 6113). G.D. Searle, one of the early manufacturers of oral contraceptives, went so far as to ‘vote away’ the risk of thrombosis at a medical conference (NPH pages 6108-6133). Sales and marketing materials were designed to dismiss the risk and obfuscate the research (NPH pages 6218-6296). This led American doctors, researchers, and the population as a whole, to presume falsely that the pill was safe and without risks. It bears noting that by failing to publish the evidence implicating the pill in thrombosis and by allowing industry experts to write and publish the safety reports, the American Medical Association set the precedent for what has now become a complete abrogation of scientific and medical ethics, not only regarding contraceptives, but also, for every other drug on the market.
Beyond Thrombosis: System Wide Side Effects
A persistent notion in contraceptive research is that progesterone and estradiol, the two hormones mimicked in contraceptives, are singularly involved with reproduction. What follows is a presumption that these hormones have no impact on other tissues and altering them affects nothing but the intended target. Contrary to this popular belief, these steroid hormones are not solely involved in reproduction. Hormone receptors are distributed throughout the brain and the body, on every organ, in every tissue, and in every fluid. Hormones, thus, regulate every physiological system. When synthetic hormones bind to endogenous or native hormone receptors, they effectively override the body’s natural regulatory functions in ways we have yet to comprehend fully. It is not unexpected then that the use of hormonal contraceptives would have broad based effects. Thus, in addition to the higher incidence of thrombotic events in otherwise healthy women, physicians and researchers testifying at the hearings noted clear associations between the use of hormonal contraceptives and a broad array of disease processes. Some of those effects are highlighted below.
Metabolic Disturbances
Perhaps some of the least well-recognized effects of these hormones include those to a woman’s general metabolism. Hormonal birth control induces wide ranging metabolic disturbances in insulin and glucose regulation, lipid control, and in heart rate, rhythm and pressure leading to weight gain, diabetes, high blood pressure, and cardiovascular disease. One researcher testified accordingly:
And yet another said:
Impaired Reproductive Capacity
Impaired reproductive capacity, likely due to the pill’s effects on the pituitary gland and its ability to prevent ovulation was noted (Dr. James Whitelaw, NPH pages 6009-6019). Case studies presented by the physicians indicated use of hormonal birth control often delayed fertility while the body re-adjusted to its non-pill state. In at least 1-2% of the women who used the pill, however, it caused permanent infertility. Ovulation never resumed. Additionally, women who used the pill were more prone to miscarriage, stillbirth, and chromosomal abnormalities in the offspring; abnormalities that as one researcher indicated were:
Sadly, much of this research was disregarded and there has been very little work since. In fact, the use of oral contraceptives to regulate cycles in advance of fertility treatment is now commonplace. Despite research suggesting it is contraindicated.
Beyond the immediate effects to fertility and reproduction, early researchers postulated potential transgenerational effects. That is, when women use hormonal contraceptives, ovulation is suppressed unnaturally and germ cell damage to the ovarian follicles is possible: damage that may not only express itself in the first generation, but also in subsequent generations, e.g. in her grandchildren and great grandchildren.
Cancer
One of the most damning, but again disregarded and disputed, findings of the early researchers was the association between hormonal birth control and cancer. Researchers testifying at the Nelson Pill Hearings noted that cancer developed in all animal models tested when oral contraceptives were administered. In fact, the use of synthetic estrogens is banned in animal husbandry in Europe because it causes cancer in the animals and also in the workers. In the US, there is no such ban, owing partly to the decades delay in cancer onset but mostly to industry lobbying.
Liver
Liver function, because of its role in drug metabolism and detoxification, is inevitably altered by the use of any medication. To what extent the liver is impacted, is a key safety issue reviewed during drug approval considerations. As one might expect, hormonal contraceptives degrade liver function. At the hearings, researchers testified to four key changes in liver function.
Overall, the changes in liver function were summed up as follows:
We have yet to answer the question of permanent damage, although a large study in 1997 suggests that liver damage abates upon cessation.
Disturbed Immune Function
One of the most commonly recognized but simultaneously disregarded effects of hormonal contraception include disturbances in immune function. Autoimmune diseases such as lupus and rheumatoid arthritis are significantly more common in women than men, especially in women who use hormonal contraceptives. Once again, the onset and increased incidence post-pill use was noted as soon as these medications hit the market, but because of the complexity of these diseases, all but disregarded. Early researchers noted that with new onset cases once contraceptive use ceased, symptoms resolved and most patients remained symptom free for at least the 2.5 years of the study period (Dr. Giles Boles, NPH pages 6086-6108). In recent years, awareness of this connection has increased somewhat.
In addition to the increased incidence of autoimmune diseases associated with hormonal contraception, other immune system changes were noted, and again, dismissed.
Namely, the use of hormonal contraception increases the incidence of bacterial and fungal infections and the risk for developing sexually transmitted diseases. More recently, researchers have identified the mechanisms by which contraceptives initiate these disease processes – via changes in cervical immune composition that increase a woman’s vulnerability to infection. Hormonal contraceptives also predispose women to persistent MRSA infections.
Psychiatric Illness
Perhaps one of the more disturbing findings regarding hormonal contraceptives is their role in new onset psychiatric illness and their capacity to induce suicide. In the original trials, at least one women committed suicide while taking the pill. Her case, along with at least 18 other deaths (Dr. Edmond Kassouf, NPH pages 6108-6133), was omitted in the reports filed to the FDA.
Despite the early research, connections between hormonal contraceptives and mental health have been largely ignored. In fact, since the nineties, hormonal contraceptives have been marketed specifically for depression and anxiety in direct opposition to the data suggesting these medications cause and/or exacerbated psychiatric illness. As recently as three years ago, an epidemiological study suggested,
Fortunately, the tide appears to be changing. Fifty years after the release of these medications and after generations of women have complained of serious mental health issues while using hormonal contraceptives, a large study published definitive data indicating that hormonal contraceptives did indeed induce depression, especially in adolescents. No doubt, industry sponsored studies will surface shortly and contradict these findings.
Hormonal Contraceptives Today
Today, 80% of American women will use hormonal contraception at some point in their lives, mostly oblivious to their risks for thrombosis or any other of the side effects. Indeed, most women and physicians consider the side effects extremely rare, if they consider them at all. This is largely due to the fact that the American College of Obstetrics and Gynecology and other medical associations routinely claim they are safe. At any given time, 62% of women of reproductive age are using at least one contraceptive method. In contrast to the perceived lack of side effects, the numbers tell a different story. Fully 60% of women will cease using hormonal birth control within six months of initiation because of side effects and 30% will try up to five different types of hormonal contraceptives, switching between brands to temper side effects. Given that most brands may vary in name only, switching between brands is often a fruitless endeavor, something prescribing physicians seem not to appreciate.
That there are over 200 brands currently available on the market worldwide, suggests an abundance of options, but from a pharmacological standpoint, not much has changed in hormonal contraceptive technology over the last half century. The predominant estrogen used in contraceptives remains the same as was developed decades ago, a compound called ethinyl estradiol (EE2). With the exception of the fourth generation progestins, the progestins used in modern contraceptives involve only slight modifications to the original compounds. Even the ‘newer’ delivery methods, like the intrauterine device and the cervical ring, were developed decades ago, in the 1950s and 1960s. For all practical purposes, contraceptive technology remains as it was over half a century ago. Therefore, today’s contraceptives carry as many or more of the side effects and risks as their predecessors did.
Only now, our increased familiarity with these drugs has fostered a deeply ingrained but false sense of safety. Phrases suggesting that after 50 years on the market these are among ‘the most studied medications’ pepper the literature. When in fact, these medications were never studied properly before their release:
And they have not been studied conclusively since. For all intents and purposes, safety issues associated with hormonal birth control remain largely under-investigated and unrecognized. What research exists generally favors commercial interests, and if we’re honest, our interests as women. We want easy, safe and effective birth. We need it and so we ignore the side effects and ignore any research that confirms our suspicions. We allow ourselves to accept the risks. Maybe it’s time we didn’t. Maybe it’s time we dig in and find out what is really going on and then fix the problems.
Share your Story
If you have a birth control story, please consider sharing it on Hormones Matter.
Posted in News & Commentary | No Comments »